Handling a patient is an easy task. You diagnose them and give them the right treatment. Underneath that healthcare journey is a complex network of codes, claims, and approvals. While these aspects are critical, they are mostly overlooked as part of the medical billing process.
The U.S. medical billing process is like the foundation of healthcare practice. Converting patient services into financial reimbursements requires a step-by-step approach. Any error can introduce the risk of claim denials and delayed payments, which can have a huge impact on revenue.
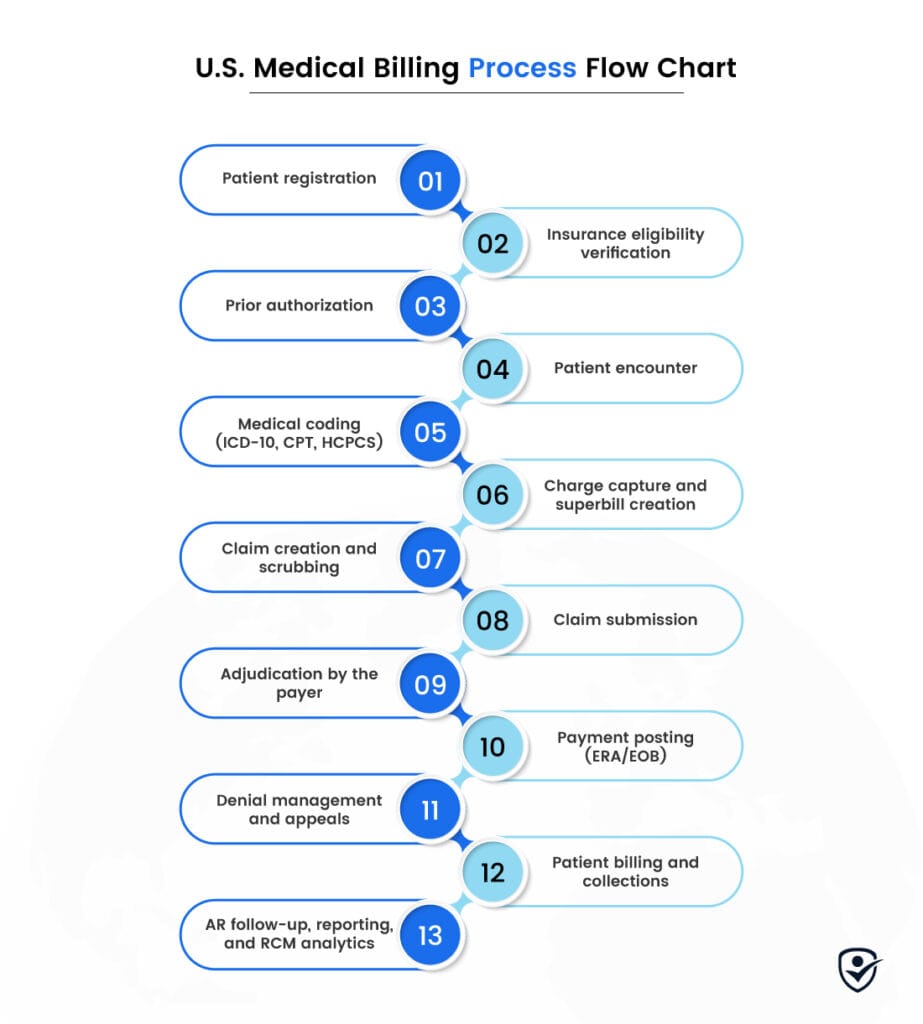
You’ll better understand how this medical billing process works with a flowchart visual by examining each stage, from initial patient contact to the final step.
What is the Medical Billing Process
The medical billing process acts like a communication channel between healthcare providers and the patient’s insurance company. This workflow is known as Revenue Cycle Management (RCM).
So, it starts with a patient making an appointment. It ends when the provider has received full payment for their services. The process overall involves the patient, the healthcare provider, and the payer (insurance company or government body like Medicare or Medicaid).
Medical Billing Cycle Flow Chart: Step-by-Step Breakdown
Implementing a medical billing process is crucial to provide much-needed stability for healthcare practices. It’s a 13-step approach:
Step 1: Patient registration and demographic capture
The RCM cycle starts with patient registration. In this process, demographic (age, name, contact, gender) and insurance information (insurance company and policy number) are needed.
If there are errors in patient registration, such as an incorrect date of birth or a missing digit in the policy number can lead to claim rejection. This step is crucial because correct information helps avoid delays and claim issues.
Step 2: Insurance eligibility verification
Once the healthcare team gets demographic and insurance details of the patients, they check whether the patient‘s insurance coverage is active or not and what it covers. They also check whether pre-authorization is required. This step is important for hospitals because you can know whether the services you are providing will be reimbursed.
Practices end up writing off services when they cover the services that patients’ insurance never covered. It happens when they do not conduct proper insurance verification. It often stems from incomplete medical documentation, which creates compliance risk and gaps in the revenue cycle.
To avoid such mistakes, make sure you check:
- Eligibility before 24-48 hours of appointments
- Check whether referral or insurance approval is required
- Document all the information you got from the insurance company and the source of confirmation
Step 3: Prior authorization
Healthcare practices are required to get approval from insurance companies before performing treatments, such as surgeries and scans. This approval is called pre-authorization. If this approval is not obtained, the insurance may refuse to pay the claim, which can delay or reduce reimbursement.
New CMS Interoperability and Prior Authorization Final Rule was finalized in January 2024. It states faster mandates and electronic authorization processing by 2026. It impacted payers. They must adhere to 72-hour limits for urgent requests and 7 days for standard requests.
Step 4: Patient encounter and clinical documentation
Healthcare providers note everything, including diagnostic tests, treatment, tests performed, and the medical reasoning after a patient visits. This document becomes the basis for an insurance claim.
CDI programs are important because insurers now use AI tools to review medical records. They also detect unclear or weak documentation with the help of these tools. So, write the diagnosis and medical necessity carefully to avoid any claim denials.
Step 5: Medical coding (ICD-10, CPT, HCPCS)
Medical records are converted from the providers’ notes into billing codes. These billing codes help insurance companies know about the diagnosis and treatment provided to patients.
- CPT code describes procedures
- ICD-10 codes represent diagnosis
- HCPCS codes cover medical supplies, equipment, and other related services
Coding mistakes are one of the main reasons claims get rejected. Common issues include unbundling, upcoding, and downcoding, missing required modifiers, and incorrect evaluation and management (E&M) level selection.
In many cases, these issues are escalated when EHR systems fail to provide patient medical history across systems. It leads to missing or incomplete patient data during coding.
Step 6: Charge capture and superbill creation
This is the process where all coded services are entered into billing systems and given a price so clinics can get paid. This step makes sure every service provided during a patient visit is properly recorded for billing.
If the process is slow, your healthcare practice can face a delay in the billing process and may miss the insurance company’s claim submission deadline. To avoid these issues, healthcare practices should implement audit trails to track every charge.
Step 7: Claim creation and scrubbing
Billing details are added to the insurance claim form at this stage. Before sending this claim form, hospital staff check their form using claim-scrubbing software to identify any mistakes before submission. After identifying errors, they can easily remove them.
The common issues that can reject claims include missing modifiers, incorrect NPI numbers, or a mismatch between diagnosis (ICD) and procedure (CPT) codes. So, make sure you submit clear and error-free claims to get paid quickly for the services provided to the patients.
Step 8: Claim submission (clearinghouse or direct)
After scrubbing, you send the claim form to the insurance company electronically. This claim form usually goes through a clearinghouse. It acts as a messenger and checker between the healthcare providers and the insurance company.
The clearinghouse reviews the claim to make sure it is well-formatted and then sends it to the insurance company. The claim is sent in standard digital formats:
- 837P for doctor or clinic (professional) services
- 837I for hospital (institutional) services
If you send this claim form to the wrong insurance company or send it in an incorrect format, your claim will be rejected. So, make sure to check the clearinghouse reports carefully and fix any errors before resubmission.
Step 9: Adjudication by the payer
After insurance companies receive the claim, they check it and decide how much they will pay to providers. Insurers check:
- Service covered or not
- How much reimbursement is allowed
- Policy rules are met or not
The results can be a full approval, partial approval, or a request for more information. You can get this outcome through Explanation of Benefits (EOB) or Remittance Advice (RA).
Step 10: Payment posting (ERA/EOB)
In this step, the billing team records the insurance payment in the system and matches it to the correct claim. It includes:
- Checking how much the insurer paid
- Applying contract-based adjustments (such as negotiated discounts)
- Identifying the remaining balance that the patient has to pay
Correct payment posting keeps all financial records clear and up-to-date. This helps avoid confusion caused by mistakes and saves time by preventing problems that would need to be fixed later.
Step 11: Denial management and appeals
After the insurance company rejects any claims, the billing team must review and resubmit the claim. They review the claim, fix the mistakes, and send it again within the given time period. According to a report, 86% of claim denials are potentially avoidable. Only 35-65% are resubmitted.
If you do not resubmit the claim within the given deadline, your claim will be rejected completely. It helps you find errors quickly and fix them.
Step 12: Patient billing and collections
After the insurance company pays its portion, the remaining balance is billed to the patient. It’s the billing team’s responsibility to send statements and follow-ups to collect the payments. Itemized digital bills help patients clearly understand the charges and usually lead to faster payments.
According to CFPB data, around 100 million Americans carry over $220 billion in total medical debt. So, clear and transparent billing is important for both compliance and patient trust.
Step 13: AR follow-up, reporting, and RCM analytics
This is the ongoing process of tracking and managing all unpaid claims to make sure revenue is collected on time. The billing team monitors key performance indicators (KPIs) like Accounts Receivable (AR) aging, denial trends, and how many claims are accepted on the first submission.
2026 Benchmarks:
- Clean claim first-pass rate: above 95%
- Accounts Receivable (AR) days: under 35 days
In simple terms, this step helps practices see how well their billing process is working and quickly fix issues that slow down payments.
2026 Changes Affecting the Billing Process Flow Chart
Several structural changes in 2026 are shaping how the medical billing process works end-to-end. These updates are not just minor changes; they directly affect how claims are checked, submitted, reviewed, and paid by insurance companies.
Several key updates make the 2026 billing landscape unique:
CMS Prior Authorization API Rule
The CMS prior authorization API rule is a 2026 health care regulation that requires insurance companies to use digital API-based systems to handle prior authorization requests.
What changed in 2026?
Before this rule | After the 2026 CMS rule |
|
|
Impact on billing flow
- Faster and authorized billing decisions
- Reduced manual intervention, but increased dependence on accurate integration
No Surprises Act Enforcement
The No Surprise Act enforcement is a U.S. law designed to protect patients from unexpected medical bills, especially for emergency and out-of-network services.
What changed in 2026?
Before this enforcement | After 2026 |
|
|
Impact on billing flow:
- Extra documentation is required for out-of-network claims
- Higher penalties for providers who charge patients incorrectly
ICD-10 and CPT Code updates
On January 1, 2026, the American Medical Association (AMA) announced the release of 288 new CPT procedure codes. Similarly, on October 1, 2025, 487 new ICD-CM diagnosis code updates were implemented.
These codes address the latest advances in medical, surgical, and diagnostic services, allowing a smooth flow of complex information across the entire health system.
What changed in 2026?
Before | After |
|
|
Impact on billing flow:
- If old or incorrect codes are added, claims will be denied
- Codes need regular training to stay updated
Conclusion: Building a Denial-Resistant Revenue Cycle
Medical billing is more automated and data-driven in 2026. But the main problem is still errors in documents submitted to insurance companies. Common reasons behind claim denials are errors in registration, coding, and prior authorizations.
With stricter CMS rules, preventing errors is more important than fixing them later. You can catch errors early when you have tools to get accurate information about the patient from the beginning.
Healthcare practices are increasingly leveraging virtual medical billing assistants and revenue cycle specialists to strengthen accuracy, reduce denials, and improve overall cash flow. So, if you want to ensure a smooth medical billing process, ensure every step is implemented accurately.
Most Frequently Asked Questions
What are the steps in the medical billing process?
The medical billing process includes: 1. Patient Registration, 2. Insurance eligibility verification, 3. Prior authorization 4. Patient encounter and clinical documentation 5. Medical coding (ICD-10, CPT, HCPCS) 6. Charge capture and superbill creation 7. Claim creation and scrubbing 8. Claim submission (clearinghouse or direct) 9. Adjudication by the payer 10. Payment posting (ERA/EOB) 11. Denial management and appeals 12. Patient billing and collections 13. AR follow-up, reporting, and RCM analytics
What is the difference between medical billing and revenue cycle management?
Medical billing is the process that involves the creation and submission of claims to insurance companies for services providers render. Revenue Cycle Management (RCM) is the financial process utilized by healthcare systems to track patient care from initial appointment scheduling to final payment collection.
How long does the medical billing cycle take from claim to payment?
The average medical billing cycle takes 40 to 50 days from claim submission to full payment. Highly efficient practices receive payment within 30 days. Electronic claims are paid within 14-30 days.
What causes the most claim denials in medical billing?
The main causes of medical billing claim denials are registration errors, coding errors, missing prior authorization, eligibility issues, and timely filing violations.
What are the new CMS rules affecting medical billing in 2026?
The new CMS rules that affect medical billing in 2026 are interoperability and prior authorization API rules, which require payers to use digital systems for a fast prior authorization process. Additionally, ICD-10 and CPT codes and the No Surprises Act Enforcement are also enforced strictly.
How does prior authorization fit into the billing process flow chart?
Prior authorization occurs after insurance verification but before the patient’s visit. It’s like a gatekeeping step where insurers approve certain services in advance, such as surgeries. Without this approval, the claim can be denied.


